Confused by Healthcare Insurance Terms? Let’s Simplify Out-of-Pocket Costs
In the world of healthcare insurance, navigating terms like out-of-pocket maximum, deductibles, and coinsurance can feel overwhelming for both patients and practice managers. Understanding healthcare insurance terms like these is essential when selecting a plan through the health insurance marketplace or managing medical expenses.
- Confused by Healthcare Insurance Terms? Let’s Simplify Out-of-Pocket Costs
- What does out-of-pocket mean?
- How does an out-of-pocket maximum work?
- What costs contribute to this maximum?
- What is not included?
- What Will Happen When the Out-of-Pocket Maximum is Met?
- Common Questions Patients Should Ask Their Insurance
- Texas-Specific Note: Why It Matters
- Conclusion
What does out-of-pocket mean?
The out-of-pocket maximum is the total amount you must pay for covered healthcare services in a given plan year. Once you reach this limit, your health plan will cover 100% of the covered costs for the remainder of that year.
If you desire to have members of the family on your plan, you can have individual out-of-pocket maximums and a family out-of-pocket maximum based on the terms of the health plan.
- Individual Out-of-Pocket Maximum: This is the maximum amount that an individual on the plan will have to pay for their covered healthcare services in a plan year.
- Family Out-of-Pocket Maximum: This is the maximum amount that all family members combined will have to pay for their covered healthcare services in a plan year.
How does an out-of-pocket maximum work?
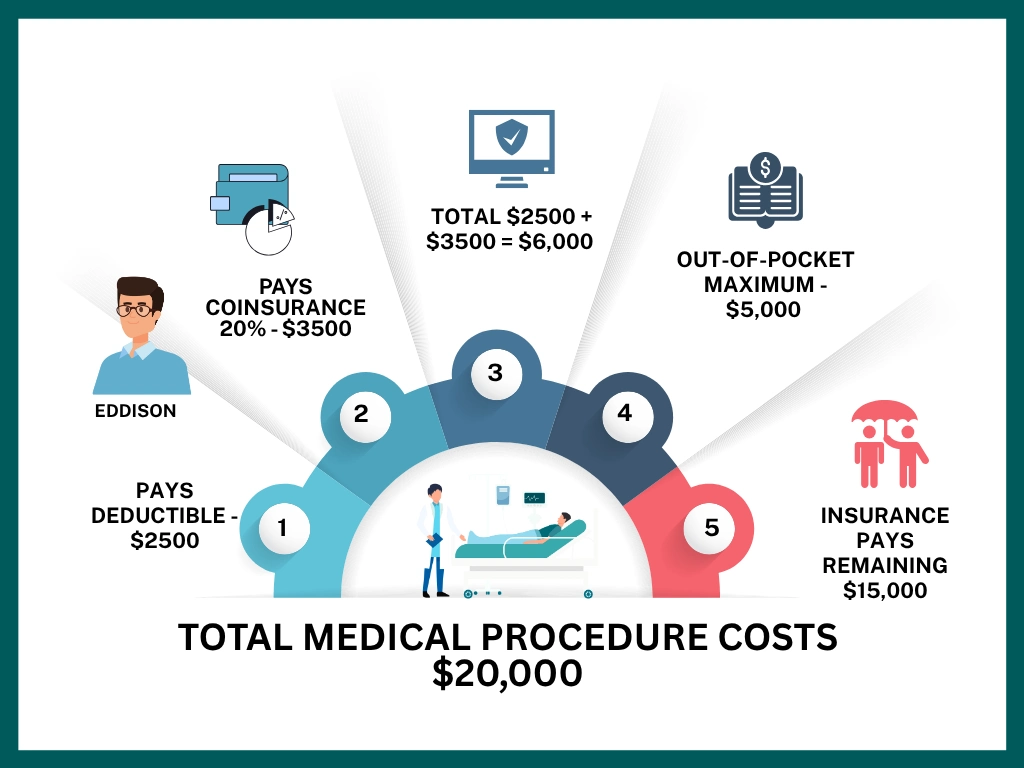
Eddison needs to undergo a medical procedure that costs $20,000. Concerned about the financial burden, he wants to ensure he receives the maximum coverage for the expenses.
- Eddison has a health insurance plan with the following:
- Deductible – $2,500
- Coinsurance – 20%
- Out-of-pocket maximum – $5,000
- In this scenario, Eddison has a medical procedure that costs $20,000. Here’s how the costs would be shared:
- Deductible: Eddison pays the first $2,500.
- Coinsurance: Eddison then pays 20% of the remaining $17,500, which is $3,500.
- Total: The total amount the person pays is $2,500 + $3,500 = $6,000.
- Out-of-Pocket Maximum: However, the person’s out-of-pocket maximum is $5,000. So, the insurance pays for any covered costs over that amount.
- In this case, Eddison pays $5,000, and the insurance company covers the rest $15,000.
What costs contribute to this maximum?
Once you’ve reached the out-of-pocket maximum within your plan year through deductibles, copayments and coinsurance for in-network services, your insurance will share 100% of your eligible healthcare costs.
- Deductibles – are the costs you pay out-of-pocket for covered healthcare services each year before your insurance plan starts to pay its share.
- Copayments – A fixed amount you pay as part of insurance coverage for medical services.
- Coinsurance – Your share of the cost of a covered service, usually expressed as a percentage. A fixed percentage of your share towards the cost of a covered medical service after a deductible is met.
What is not included?
There are several expenses that may not be included in the out-of-pocket maximum:
- Preventive care: Preventive care services (annual check-ups, routine vaccines) are often covered at no cost to individuals when received from an in-network provider under ACA-compliant plans and does not contribute to the maximum. However, if a preventive service results in additional testing or treatment, any related copayments or coinsurance will be applied to your expenses.
- Premiums: Your regular monthly premium payments for your insurance coverage are not included in the out-of-pocket maximums. You are required to keep paying the premiums even if the maximum out-of-pocket limit is reached.
- Costs for non-covered services: These are the expenses for treatments or services that your health insurance plan doesn’t cover. Therefore, you are obligated to pay expenses for non-covered services which will not contribute to reaching your out-of-pocket maximum. Example – cosmetic treatments.
- Out-of-network costs: The in-network providers agree to provide their services at discounted rates to the health plan customers. If you wish to see an out-of-network provider, your medical costs may not be shared by insurance, though some plans may offer to cover a portion. The costs for out-of-network care do not contribute to your out-of-pocket maximum.
- Balance billing: This happens when you go to out-of-network providers, and they bill you for the difference between their charge and the amount your insurance pays. The balance amount that exceeds the allowed limit is typically not considered a covered expense.
What Will Happen When the Out-of-Pocket Maximum is Met?
Once you meet your out-of-pocket maximum within a plan year, your insurance coverage changes:
- 100% Coverage: Your health insurance plan will then fully cover the allowed costs for covered healthcare services for the rest of that plan year.
- No More Cost-Sharing: Typically, you won’t need to pay any more deductibles, copayments, or coinsurance for covered services until the plan year ends.
Common Questions Patients Should Ask Their Insurance
If you’re choosing a new health plan or unsure about your current benefits, ask your insurance provider these key questions:
- What’s my individual out-of-pocket maximum and how much have I met so far this year?
- Are preventive care services covered at no cost?
- What happens if I see an out-of-network provider?
- Will I face balance billing charges for out-of-network care?
- Does my plan offer cost-sharing reductions if I qualify through the health insurance marketplace?
These answers can help you better predict medical costs and avoid unexpected bills.
Texas-Specific Note: Why It Matters
In Texas, U.S., to make healthcare more affordable for individuals and families with lower incomes, cost-sharing reductions are designed. These reductions help decrease their out-of-pocket maximums. To be eligible for cost-sharing reductions, individuals and families must:
• Meet certain income requirements.
• Enroll in the Silver category health plan on the Health Insurance Marketplace.
Conclusion
The out-of-pocket maximum generally represents the maximum amount you’ll pay for covered healthcare services in a health plan year. Familiarizing yourself with this concept, along with other cost-sharing elements, can help you make informed decisions that align with your health and financial circumstances.
Need help decoding your health insurance marketplace options or clarifying your out-of-pocket cost limits? Call our team at Integrate Point, we simplify coverage decisions for clinics and patients across Texas.



