Prior authorizations are costing Texas clinics time, revenue, and staff morale. This guide shows proven fixes you can start this week.
- Texas Clinics Can Streamline Care Without Getting Stuck in the Prior Auth Delays
- What is Prior authorization?
- Why Prior Authorization Delays Hit Everyone – Clinicians & Patients
- The Hidden Cost of Delays
- Why Prior Authorizations get stuck
- Smart, Actionable Steps to Minimize the Bottleneck
- The Payoff: What Your Clinic Gains
- The Patient Experience Matters
- Final Thought
Texas Clinics Can Streamline Care Without Getting Stuck in the Prior Auth Delays
If you’re running or working in a clinic in Texas, you’ve likely experienced the frustration of prior authorizations (PAs). You’re ready to deliver care; your patient is ready for treatment, but the insurance says, “Not so fast.” Suddenly, you’re caught in a web of paperwork, phone calls, and portal logins, all before a procedure or medication can move forward.
What is Prior authorization?
Prior authorization is the approval that healthcare providers must obtain from insurance companies before delivering certain treatments, services, or medications. While intended to control costs and ensure appropriate care, this process can create major administrative slowdowns.
There are smart, actionable ways to streamline your internal workflows and reduce the bottlenecks even while larger policy fixes are still pending.
In this blog, we’ll explore how clinics can take proactive steps to minimize the friction caused by prior auth delays and keep their operations running smoothly.
Why Prior Authorization Delays Hit Everyone – Clinicians & Patients
For Clinics and Hospitals:
- Bottlenecks in workflow delay downstream services, rescheduling, or referral chains.
- Staff time gets swallowed in chasing approvals instead of delivering value.
- Cash flow stalls when authorizations linger or claims are denied.
- Morale and burnout rise when administrative overhead swallows clinical time.
For Patients:
- Longer wait times for tests, medications, or treatments.
- Frustration, confusion, and trust erosion.
- Some patients abandon or skip care when delays drag out.
- Perception that the system is unresponsive or dismissive.
The Hidden Cost of Delays
Let’s be honest, prior authorizations aren’t just annoying.
- 93% of physicians report that prior authorizations delay access to necessary care (AMA).
- Clinics can spend 13 hours per week per physician managing authorizations – that’s clinical time diverted to paperwork.
For small to mid-sized clinics, especially in fast-paced areas like Dallas or Houston, these delays create bottlenecks that hit both morale and the bottom line, that often looks like:
- Longer wait times for patients
- Cancelled or rescheduled appointments
- Reduced staff productivity
- Interrupted revenue cycles
Why Prior Authorizations get stuck
Most delays trace back to a few recurring problems:
- Incomplete submissions: missing ICD/CPT codes, incorrect NPIs, or absent clinical notes will trigger rejections.
- Payer’s variability: each insurer has different rules; what’s acceptable for one is denied by another.
- Manual workflows: faxes, phone calls, and spreadsheet tracking are slow, and error prone.
- Poor escalation paths: no clear way to prioritize urgent requests or follow up efficiently.
- Lack of feedback and pattern tracking: You don’t know which payers are consistently slow or which denials repeat.
Understanding the root causes is the first step toward fixing them.
Case Example
A mid-sized clinic in San Antonio discovered that 40% of their PA requests were rejected because of missing clinical notes or mis-matched provider credentials. After tracking, they cut their average turnaround from 4.2 days to 1.8 days within two months.
Smart, Actionable Steps to Minimize the Bottleneck
While we may not be able to eliminate prior authorization altogether, we can certainly make the process smoother.
1. Ensure Pre-Submission Accuracy and Completeness
The fastest way to get a “denial” or a “delay” is an incomplete submission. Think of your prior auth request as a critical legal document – every detail matters.
- Standardize Documentation: Before sending any request, ensure patient details, provider NPIs, facility info, CPT, and ICD-10 codes are accurate. Simple typos can trigger immediate rejections.
- Payer-Specific Requirements: Train your staff to understand the unique requirements of different insurance companies. Each insurance company has unique criteria; what’s approved by one may be denied by another.
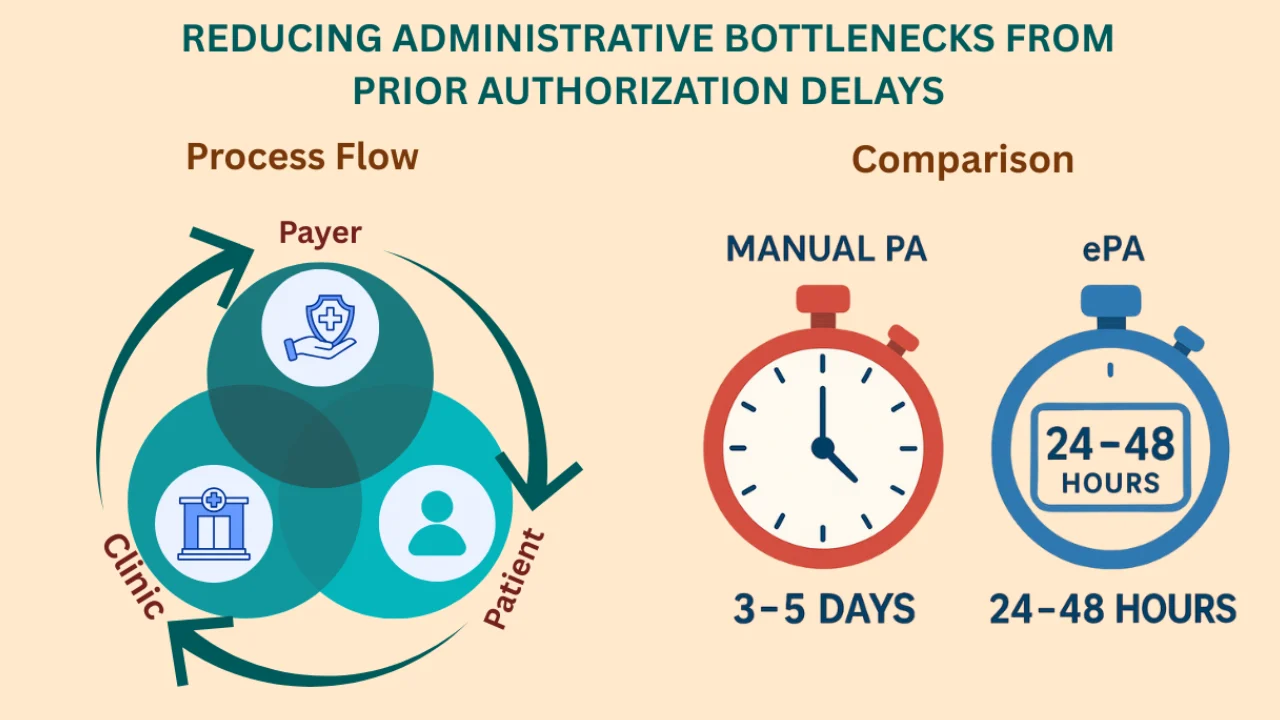
2. Automate and Technology
Use digital platforms and clearinghouses that enable electronic prior authorization to speed up approvals and reduce manual work.
Many insurers in Texas now support real-time PA through platforms like:
- Availity: widely used by BCBS and major payers
- CoverMyMeds: simplifies prescription PAs and integrates with many EHRs
- Surescripts: enables real-time PA and data sharing
These can drastically cut down processing time, manual effort, and submission errors.
3. Train & Cross-Train Your Team
Instead of scattering PA responsibilities across multiple staff members, assign a dedicated staff member (or a small team) or billing partner who’s well-versed in prior auth requirements is gold.
But training your front desk or nursing staff to recognize PA flags can stop delays before they begin. This builds consistency, accountability, and expertise.
4. Outsource the Hassle
Many small clinics in Texas are turning to medical billing and credentialing support partners or virtual assistant companies who handle authorizations end-to-end. This lets your team stay focused on care, not on hold.
These companies often have dedicated teams and advanced technology to handle the process efficiently and compliantly.
Benefits include:
- Expert teams that stay current on payer rules
- Faster submission turnaround
- Reduced staff workload
This approach lets your team focus on patient interaction instead of waiting on hold with insurers.
5. Monitor Turnaround Times
Set up a flagging system in your EHR or patient scheduler for urgent authorizations. Track how long each payer takes to respond. Over time, this data can help identify consistent, slow responders.
You can then:
- Escalate chronic delays
- Adjust scheduling based on typical approval timelines
- Strengthen future payer contract negotiations
6. Track and Flag Urgent Requests
Set up a flagging system in your EHR or patient scheduler for time-sensitive authorizations (e.g., imaging, specialty referrals).
Prioritize these daily and follow up more aggressively to reduce care delays and patient frustration.
7. Build an Appeal and Denial Log
Maintain a history of PA denials, appeal results, and payers’ feedback. Over time, this gives you insight:
- Common denial reasons
- Which payers require more documentation
- Which procedures need preemptive evidence
This data helps your staff improve accuracy and reduce repeat errors.
8. Foster Proactive Communication:
- Patient Education: Educate patients early about the prior auth steps and possible waiting periods; this helps set clear expectations and eases concerns.
- Payer Communication: Develop strong lines of communication with your top insurance partners. Know their preferred submission methods and follow-up guidelines.
The Payoff: What Your Clinic Gains
By proactively addressing prior authorization delays, your Texas clinic can experience significant benefits:
- Faster Reimbursements: Streamlined processes mean quicker approvals and a healthier revenue cycle.
- Improved Patient Satisfaction: Patients receive timely care, leading to better outcomes and a more positive experience with your clinic.
- Lower Administrative Costs: Cutting down on manual processes helps reduce admin workload—and brings down your clinic’s overhead costs.
- Empowered Staff: Free your team from repetitive, frustrating tasks, allowing them to focus on higher-value activities and direct patient interaction.
- Healthier cash flow: Fewer claims stuck in pending status = more reliable revenue.
The Patient Experience Matters
Remember, patients don’t always understand the “why” behind delays; they just know they’re waiting. Transparent communication and reducing back-office delays can improve trust, satisfaction, and retention.
Simple strategies like email updates, patient portal notifications, or text alerts can ease anxiety and reduce inbound calls to your staff.
Final Thought
Prior authorization may be a necessary part of modern healthcare, but it doesn’t have to stall your clinic’s operations.
By combining technology, staff training, smart outsourcing, and strong payer relationships, you can minimize the red tape and keep care flowing smoothly.
Need help optimizing your clinic’s prior authorization and billing workflow?
At Integrate Point, we help Texas-based providers streamline credentialing, payer contracting, and revenue cycle management. Our HIPAA-compliant workflows and end-to-end support ensure your clinic spends less time chasing approvals and more time caring for patients.



