Think about the last patient who missed a follow-up and never rescheduled. Someone called the front desk four times asking the same medication question. Another one showed up without the documents they needed. A referral went out and that patient just went completely silent after that.
None of those situations happened because the patient did not care. They happened because the communication between the practice and the patient broke down somewhere. The reminder did not go out. The message was not clear. A follow up never came.
Patient communication in healthcare is where outcomes are won or lost long before the patient ever steps into the exam room. And right now, virtual assistants are changing how that communication works in ways that are faster, more consistent, and more effective than anything a stretched front desk team can deliver alone.
Why Patient Communication Breaks Down in the First Place
Most practices want to communicate well with their patients. The problem is not intentional. It is a capacity. A front desk coordinator managing check ins, phone calls, insurance verification, and scheduling all at once cannot also send personalized follow up messages to every patient who missed an appointment last week.
Something always gets deprioritized. And in most practices, proactive patient communication is the first thing that falls off the list when the day gets busy.
According to AHRQ, poor communication between healthcare providers and patients is one of the leading contributors to medication errors, missed follow ups, and preventable readmissions across US healthcare practices. The cost of that communication gap is measured not just in revenue but in patient outcomes.
Virtual assistants in healthcare close that gap without adding headcount. They handle the consistent, repetitive communication tasks that matter enormously to patients but drain staff time when done manually.
What Virtual Assistants in Healthcare Actually Handle
The term virtual assistant means different things in different contexts. In healthcare, a virtual assistant is a trained remote professional or an automated communication system, or often a combination of both, that manages patients facing communication tasks on behalf of the practice.
The range of what they handle is broader than most clinic managers expect when they first consider the option.
Appointment reminders go out automatically at exactly the right time. After every visit, follow-up messages check in on how the patient is doing. Prescription refill requests route straight to the right person without anyone sitting on hold. Test results reach patients fast and in plain language. Post-discharge instructions actually make sense to patients, so they follow through.
According to HealthIT.gov, practices that use automated patient communication tools report measurable improvements in appointment adherence, follow up completion rates, and overall patient satisfaction scores. The data consistently points in the same direction. When patients hear their practice more consistently, they engage more reliably.

How Patient Engagement Solutions Change the Dynamic Between Practice and Patient
There is a difference between a practice that communicates with patients and a practice that engages them. Communication is one way. Engagement is a conversation.
Patient engagement solutions built around virtual assistants create two ways dynamic. Instead of just sending a reminder, the system sends a reminder and captures the patient’s response. Instead of just delivering discharge instructions, it follows up two days later to ask whether the patient has questions or concerns.
Consistent, responsive communication actually matters more than most clinics realize. Patients who feel heard show up. They take their medications, complete their follow-ups, and call the practice first when something feels off instead of heading straight to the ER.
According to CMS, patient engagement is directly tied to quality reporting metrics and value-based care performance scores across US healthcare organizations. Practices that invest in structured patient engagement solutions see measurable improvements in clinical outcomes that drive reimbursement rates.
For Texas practices navigating value-based care contracts, that connection between patient engagement and financial performance is not abstract. It shows up directly in the numbers.
Healthcare Workflow Automation: Where Efficiency and Communication Meet
The biggest thing clinic managers always bring up is time. Sending personalized messages to every single patient just isn’t realistic. Chasing down every missed appointment takes time nobody has. Checking whether every patient actually understood their post-visit instructions? That’s a full-time job on its own.
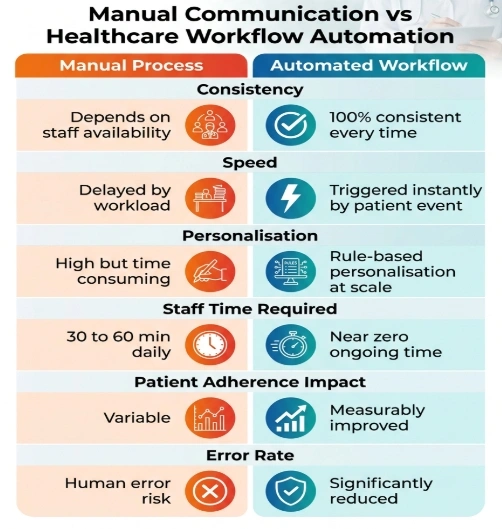
Healthcare workflow automation removes the time constraint entirely. When communication tasks are built into automated clinical workflows, they happen without anyone needing to remember to do them. The trigger is the event, not the availability of a staff member.
A patient booked an appointment. The confirmation goes out automatically. Three days before the visit, a reminder goes out. The morning of the visit, another reminder. After the visit, a follow up message. Two weeks later, a check in about the treatment plan. All of it happens without a single staff member sending a single message manually.
According to HHS.gov, healthcare automation tools that support patient communication consistently reduce administrative burden while improving patient adherence to treatment plans and follow up care. The outcome is better for the patient and more efficient for the practice at the same time.
HIPAA Compliant Communication: Non-Negotiable for Every Texas Practice
Every conversation about virtual assistants in healthcare and automated patient communication eventually reaches the same question. How do we make sure patient data is protected throughout all of this?
The answer starts with HIPAA compliant communication systems. Every message sent through a virtual assistant platform, every automated reminder, every test result notification, needs to travel through a channel that meets HIPAA security standards. That means encrypted messaging, secure portals, signed Business Associate Agreements with every technology vendor, and strict access controls on who can see what.
According to HHS HIPAA guidelines, any vendor that handles protected health information on behalf of a healthcare practice must operate under a signed BAA and demonstrate compliance with all applicable security and privacy rules. No exception.
For Texas practices especially, where the patient population is large and diverse, ensuring that HIPAA compliant communication is built into every patient touchpoint is not just a legal requirement. It is a trust requirement. Patients who know their information is protected communicate more openly and engage more reliably with their care team.
Improving Medical Practice Efficiency Through Better Communication
There is a direct line between how well a practice communicates with patients and how efficiently that practice runs. It is not always obvious at first, but the connection is real, and it shows up in the numbers.
Clear reminders mean fewer no-shows. Solid pre-visit instructions cut down check-in time. Sharing test results quickly means fewer follow-up calls coming in. Sending post-visit instructions digitally and actually following up on them keeps patients out of the hospital longer.
Each of those improvements translates directly into medical practice efficiency gains that show up in healthcare KPIs. Days in accounts receivable shorten because care is completed properly the first time. Patient satisfaction scores improve because the experience feels coordinated and professional. Staff turnover decreases because front desk teams are no longer buried in reactive communication tasks.
According to the American Medical Association, practices that implement structured patient communication programs report measurable reductions in administrative workload and significant improvements in both clinical outcomes and patient satisfaction scores within the first year.

Patient Adherence: The Outcome That Everything Else Depends On
All the technology, all the automation, all the virtual assistant infrastructure ultimately serves one goal. Getting patients to follow through on the care their provider recommends.
Patient adherence is where clinical outcomes are actually determined. A patient who takes their medication consistently, attends their follow up appointments, and follows their discharge instructions has dramatically better health outcomes than one who does not. And the research is clear about what drives adherence. Communication is at the top of the list.
According to AHRQ, patients who receive consistent, clear communication from their healthcare provider are significantly more likely to adhere to treatment plans, attend follow up appointments, and report higher satisfaction with their care experience.
Virtual assistants in healthcare make consistent communication possible at scale. Not just for the patients who happen to call in. For every single patient in the practice, every single time they need to hear from their care team.
Quality Reporting and Value Based Care: How Communication Feeds the Numbers
For practice managers navigating value-based care contracts and quality reporting requirements, patient communication is not just a patient experience issue. It is a financial and compliance issue.
Quality reporting metrics including HEDIS measures, patient satisfaction scores, and readmission rates are all directly influenced by how well a practice communicates with its patients. Practices that score well on these measures receive better reimbursement rates, stronger payer relationships, and more favorable positions in network negotiations.
Healthcare KPIs like net promoter score, appointment adherence rate, and follow up completion rate all tell the story of how well communication is working inside a practice. Virtual assistants and healthcare automation tools make those numbers measurably better by ensuring no communication task falls through the cracks.
According to CMS quality measures guidance, patient engagement and communication are core components of performance scoring under value-based care programmed across the US healthcare system.

Patient communication in healthcare means every interaction between a practice and its patients outside the exam room. Appointment reminders, follow up messages, test result notifications, discharge instructions, and prescription refill updates all fall under this category. When done consistently and clearly, it directly improves patient adherence, satisfaction scores, and clinical outcomes across the practice.
Virtual assistants handle consistent, repetitive communication tasks automatically. Reminders go out on schedule. Follow ups happen after every visit. Missed appointment outreach triggers within hours. Patients receive clear instructions in plain language. Staff are freed from manual communication tasks and can focus on higher value patient facing work.
Patient engagement solutions are tools and systems that create two-way communication between a practice and its patients. Instead of just sending messages, they capture patient responses, trigger follow up actions, and ensure no patient falls through communication cracks. Virtual assistants are a core part of modern patient engagement solutions in Texas healthcare practices.
It plugs communication directly into how your clinic already operates. Book an appointment, reminders go out. Complete a visit, follow-up messages send themselves. Spot a care gap, outreach kicks off automatically. Your staff never has to remember to send anything manually.
Every message that contains patient information must travel through HIPAA compliant channels. This means encrypted messaging systems, secure portals, and signed Business Associate Agreements with every technology vendor involved. For Texas practices, HIPAA compliant communication is both a legal requirement and a patient trust requirement that directly affects engagement and satisfaction rates.
How Integrate Point Helps Texas Practices Improve Patient Communication
At Integrate Point, we work with clinics, hospitals, and multi provider practices across Texas to build patient communication systems that are consistent, HIPAA compliant, and genuinely effective.
Our virtual assistants handle the full range of patient communication tasks so your clinical staff can focus on care rather than chasing follow ups. From appointment reminders to post visit check ins, prescription routing to care gap outreach, we build the infrastructure that keeps patients engaged and practices running efficiently.
We understand both the clinical and operational sides of patient communication in healthcare. And we know that for Texas practices, getting this right is not just about patient experience. It is about financial performance, quality reporting, and long term practice growth.
Contact Integrate Point today and let us show you what consistent patient communication looks like for your practice.



