Learn how Texas healthcare providers are cutting claim denials by 47% using prior authorization reform strategies. Save time and boost revenue with automated workflows.
How Healthcare Providers Can Stop Losing Money on Prior Authorization
The phone rings. It’s another frustrated staff member advising you that, yet another claim was denied due to a prior authorization issue. You already know what follows: hours of calls back and forth, papers shuttled from office to office, days or weeks spent waiting for someone to say yes. All the while, your team is keeping their heads above water with admin tasks, and your cash flow is suffering. If this is starting to ring a bell, you’re not the only one. Healthcare providers throughout Texas and across the U.S. are grappling with this issue. But here’s the really good news: things are ready to change.
And 2026 is when everything turns on its head. The Centers for Medicare and Medicaid Services (CMS) announced significant reforms to the prior authorization process. These changes will help alleviate your staff and drastically reduce claim denials.
At Integrate Point, we’ve been working with DFW healthcare providers as they navigate these changes, and we’ve witnessed the difference a little direction can be made, such as reducing claim denials by 47% and freeing up 15 hours per week of your team’s time. I want to explain what’s going on, and why it matters in your practice.
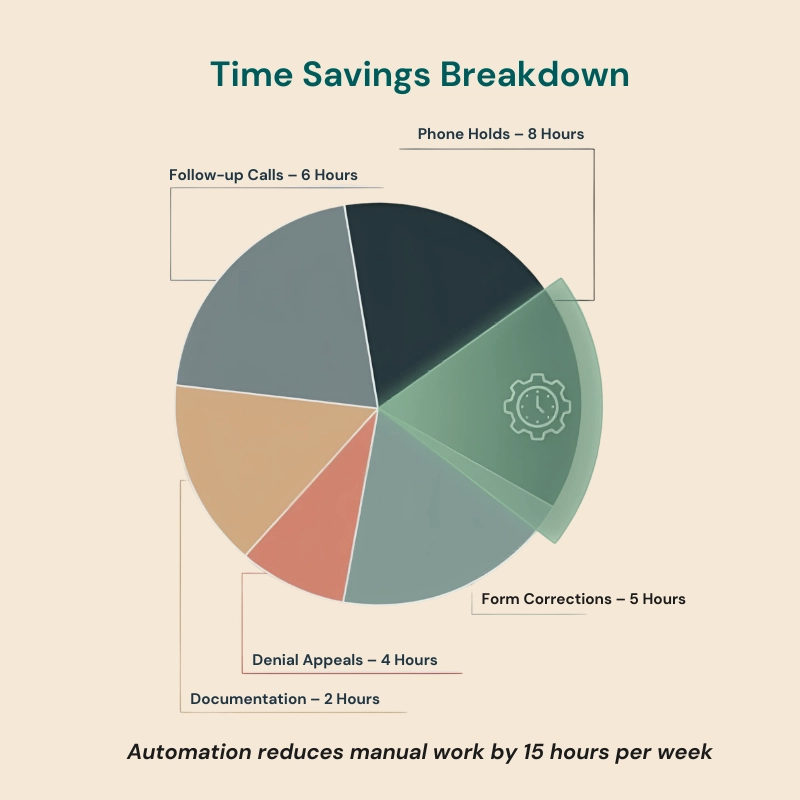
The Problem Nobody Wants to Talk About
Here’s a reality check; prior authorization isn’t just slowing you down. It costs you real money.
Think about what is happening in your clinic right now. A patient comes in, you schedule a treatment or test, and then you have to get approval from their insurance company before moving forward. Simple enough on paper, right? But in practice, it becomes a nightmare.
Your team has to call insurance companies. They wait on hold. They fill out forms. They call back because the forms weren’t filled out the “right way.” They wait some more. Some authorizations come back in days. Others take weeks. And when they do come back, maybe half of them get denied anyway, sending your team back to square one.
This isn’t just annoying. This is expensive. Each denied claim costs you time, lost productivity, and delayed revenue. Plus, your patients are frustrated because their treatment gets pushed back. Your staff is frustrated because they’re stuck playing phone tag with insurance companies instead of helping patients.

What’s Actually Changing in 2026
The new CMS prior authorization rule is a big deal. The agency finally acknowledged what healthcare providers have been saying for years: the system is broken, and it needs to be fixed.
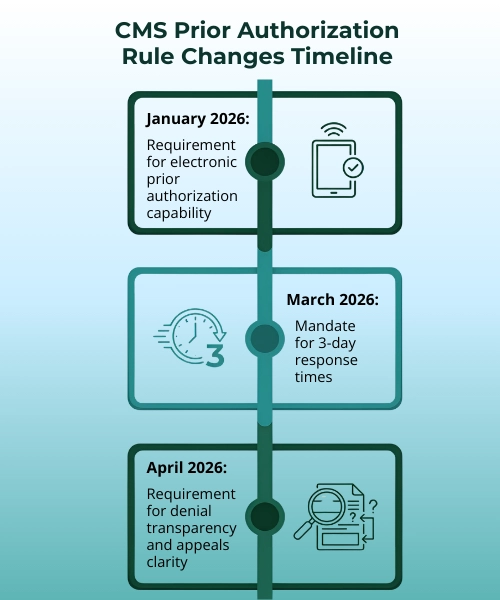
Here are the key shifts happening this year:
Insurance companies now have stricter timelines
Under the new rule, insurers must respond to prior authorization requests much faster. For most requests, they must decide within three business days. Before, this could drag on indefinitely. This alone changes the game for your revenue cycle.
Electronic prior authorization is becoming the standard
Instead of calling someone on the phone or faxing a form from 1995, you’re moving to electronic prior authorization (ePA). This means real-time submission and faster responses. No more wondering if your fax actually went through.
Transparency requirements are getting stronger
Insurance companies now have to be clear about why they’re denying a prior authorization. This helps your team understand what went wrong and how to fix it faster.
These aren’t just nice-to-haves. These changes directly impact your bottom line.
Why Electronic Prior Authorization is a Game Changer
Let’s talk about electronic prior authorization (ePA) for a second, because this is where everything gets better.
Think about what happens when you switch from calling insurance companies to using an automated prior authorization system. Your staff member no longer spends 20 minutes on hold. They don’t have to call back three times to confirm the request was received. Everything is tracked, timestamped, and documented automatically.
But here’s the really valuable part: ePA systems are smart. They can check eligibility, validate codes, and flag potential issues before you even submit. So instead of getting a denial three days later, you catch the problem and fix it immediately. Your team knows right away if something is wrong, and they can resubmit with the correct information.
At Integrate Point, we’ve seen this shift reduce claim denials by up to 47% for practices that implement it properly. That’s not a coincidence. That’s the direct result of taking the guesswork out of the process.
Building a Prior Authorization Workflow That Actually Works
So, here’s the question: how do you actually make this work in your practice?
It’s not as complicated as you might think. It starts with understanding the healthcare workflow automation opportunities you already have.
First, audit where you are right now
Look at your current prior authorization process. Where are the bottlenecks? Where do claims most often get denied? Where is your team spending the most time? Get specific about this. The numbers matter.
Second, implement the right tools
An automated prior authorization system should do three things: reduce your staff’s manual work, improve your clean claim rate, and give you visibility into what’s happening with every request. You want a system that talks to insurance companies electronically, not one where someone is still faxing forms.
Third, train your team properly
Even the best automated system won’t work if your staff doesn’t know how to use it. They need to understand the new prior authorization changes 2026 brought, what triggers a denial, and how to respond when something goes wrong.
When you put these three things together, your first-pass claim acceptance rate improves dramatically. You’re not getting denials because of missing information or incorrect codes. You’re catching those problems before they happen.
The Money Part (Because Let’s Be Honest)
Let’s get real about revenue cycle management optimization. This isn’t just about making your staff’s life easier. It’s about protecting your cash flow.
Here’s what we typically see happen when a healthcare provider moves to a better prior authorization workflow:
Your average denial rate drops significantly. Instead of 10-15% of claims getting denied due to prior authorization issues, you’re looking at more like 3-5%. For a mid-sized practice, that’s tens of thousands of dollars per year.
Your staff saves time. We’re talking about 15 hours per week for an average practice. What would your team do with 15 extra hours each week? See more patients? Actually take a lunch break? The productivity gains add up fast.
Your cash flow improves. Because you’re not spending weeks fighting denials, the money comes in faster. Your revenue cycle gets shorter. Your accounts receivable aging goes down. Banks love that stuff, by the way, if you ever need financing.
But here’s the thing that really matters: your patients get better care. Because your staff isn’t drowning in administrative work, they have time to actually focus on patient care. Authorizations come through faster, so treatment can start sooner. Everybody wins.

Making the Shift: What Healthcare Providers Need to Know
If all this sounds good but you’re wondering where to start, here’s what matters right now.
Get educated about the CMS and AMA prior authorization rule. This isn’t optional anymore. The rule is in effect. Insurance companies are already adapting. If your practice isn’t aligned with these changes, you’re already falling behind.
Evaluate your current technology
Do your systems support electronic prior authorization? Can you see which claims are pending? Do you get real-time updates, or are you still calling to check status? Honest answers to these questions will tell you how much work you have to do.
Partner with someone who understands your workflow
Healthcare operations improvement isn’t something you figure out on your own. You need partners who understand both the regulatory landscape and the practical realities of running a clinic. At Integrate Point, we work with DFW healthcare providers every day to solve exactly these problems.
Set metrics and track progress
What’s your current claim denial rate? How long does it take from submission to approval? What’s your first pass claim acceptance rate? These numbers are your baseline. Once you improve your workflow, you’ll be able to measure exactly how much impact you’ve made.
FAQs
Electronic prior authorization (ePA) uses digital systems to send authorization requests to insurers instantly instead of calling or faxing. It’s faster, more accurate, and reduces manual work because requests are automatically tracked and documented.
Most practices save 10-15 hours weekly. This comes from eliminating hold times, reducing follow-up calls, and catching errors before they cause denials. Time savings vary based on practice size and current processes.
The new CMS prior authorization rule requires insurers to respond in three business days, mandates electronic prior authorization (ePA) capability, and requires transparent denial reasons. These changes reduce delays and improve claim accuracy significantly.
Reducing denials by 47% typically adds 5-10% to net revenue depending on volume and payer mix. Combined with time savings, most practices see strong positive ROI within months of implementation.
Yes. The CMS prior authorization rule is mandatory as of 2026. Practices must either comply with electronic prior authorization requirements or face operational inefficiencies and potential compliance issues.
The Next Step
The healthcare regulatory updates 2026 presents an incredible opportunity for practices that are ready to move. The CMS prior authorization rule makes it possible to dramatically improve both your operations and your finances. But you have to actually take action.
If you’re interested in seeing how your practice compares to others and what your specific opportunities might be, that’s where we come in.
At Integrate Point, we help Texas healthcare providers do exactly this. We can audit your current process, identify where you’re losing money, and show you the path to better prior authorization workflow optimization.
The truth is simple: healthcare providers who embrace these changes early will have a significant advantage. They’ll have happier staff, better cash flow, and more time to focus on actual patient care.
The question isn’t whether you should change. It’s whether you’re ready to start.




This Post Has One Comment
Hi there! I just want to give a huge thumbs up for the great data you’ve gotten right here on this post. I shall be coming again to your blog for extra soon.