Why Verifying Insurance Eligibility Is the Step Most Practices Get Wrong
You delivered the care. Your team did everything right. And then the claim came back denied. That moment is frustrating in a way that is hard to describe. The work was done. The patient was seen. But the payment never arrived.
Most of the time, that denial traces back to one missed step before the appointment even began. That step is insurance eligibility verification. It is the process of confirming that a patient’s insurance is active and that their plan covers what you are about to provide.
This is not a complicated idea. But skipping it, even once, can cost a healthcare practice hundreds or thousands of dollars in a single week. The good news is that getting it right is entirely within your control.
Here is what solid insurance eligibility verification actually protects in your practice every single day.
Your billing stays accurate right from the get-go. Fewer claims come bouncing back rejected, which saves a ton of back-and-forth. On top of that, your whole revenue cycle just runs a lot smoother. It makes the patient’s experience smoother because nobody likes finding out their insurance did not cover something after the fact.
When patients know what their insurance covers before they walk in, everything goes smoother. No awkward billing conversations after the visit, no disputes, and no confusion. And when people feel informed and respected, they come back. They also tell others about your practice.
What Does the Process of Verifying Insurance Eligibility Actually Look Like?
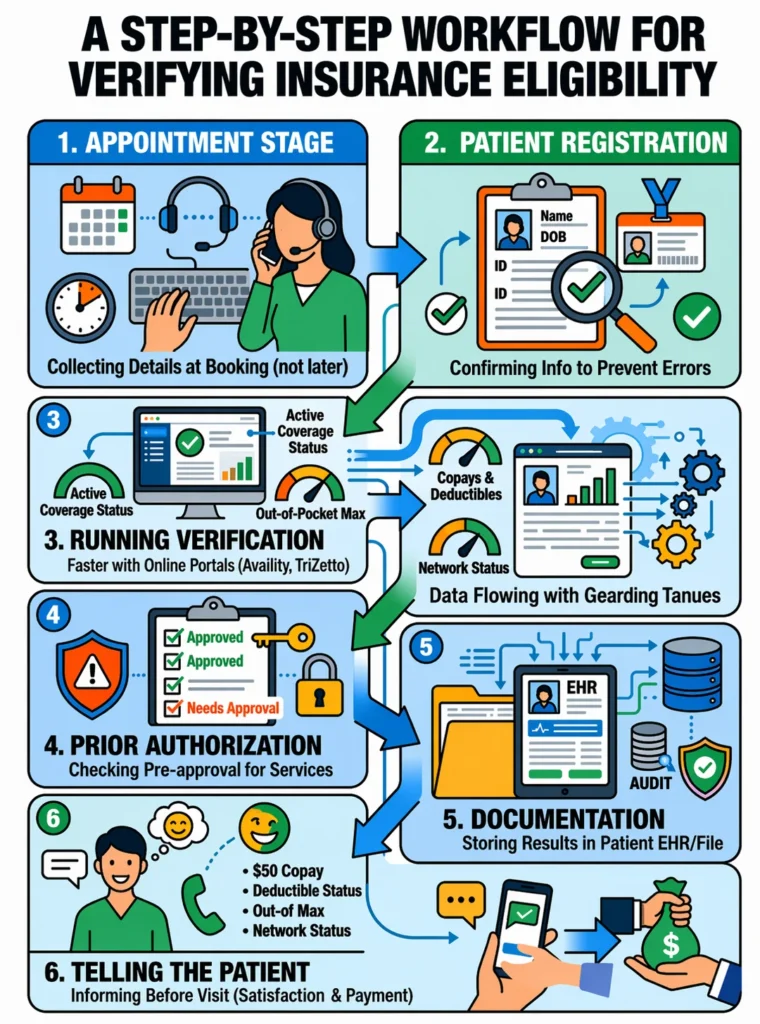
Most providers know eligibility verification exists. Fewer have a consistent, step by step process that their whole team follows every single time. Here is what that process should look like from the moment a patient calls to book.
1. It Starts at the Patient Appointment Stage
The process of verifying insurance eligibility begins the moment a patient books their appointment. Not the day before. Not at check in. Right at the booking stage. This is when your team collects the insurance details that make everything else possible.
Getting the right information early gives your staff enough time to run the check, spot any issues, and resolve them before the patient walks through the door.
2. Patient Registration Is Where the Details Get Confirmed
During patient registration, your team verifies the basic information. Name, date of birth, insurance ID, and a copy of the insurance card. These details feed directly into the eligibility check.
A small error here, a wrong digit in the member ID or a misspelled name, can cause a claim to fail weeks later. Getting it right at registration protects everything downstream.
3. Running the Eligibility and Benefits Verification
This is the core of the process. Your team checks the patient’s active coverage, the services their plan covers, their copays, deductibles, out of pocket maximums, and whether your practice is in their network.
Tools like Availity and TriZetto make this fast and accurate. You can also call the insurance customer service line directly, though that takes significantly more time. According to CMS, electronic eligibility checks are the recommended standard for reducing billing errors across healthcare services.
For most Texas practices, using an online portal is the smarter choice. It is faster, leaves a record, and reduces the chance of human error during a busy morning.
4. Checking Prior Authorization Requirements
Not every service needs prior authorization. But some do, and missing this step is one of the most expensive mistakes in the medical billing process. Before the patient is seen, your team needs to confirm whether the planned service requires approval from the insurer in advance.
The CMS Prior Authorization guidelines outline which services require pre-approval under Medicare and Medicaid plans. Checking this early keeps your claims clean and your patients moving forward without unnecessary delays.
5. Documenting Everything in the Patient File
Once the eligibility check is complete, the results go into the patient’s file or their electronic health record. According to HealthIT.gov, proper EHR documentation is a critical part of accurate medical billing and helps practices avoid repeat verification errors for returning patients.
This step protects your practice during audits and gives your billing team the information they need when it is time to submit the claim.
6. Telling the Patient What You Found
This part gets skipped more than it should. Once you know what the patient’s plan covers, tell them. Before the visit. Let them know their copay, their deductible status, and whether any prior authorization is required.
According to AHRQ, patients who are informed about their financial responsibilities before a visit are significantly more likely to pay on time and report higher satisfaction with their care experience.
Why Insurance Eligibility Verification Matters for Your Revenue Cycle
Every healthcare organization runs on cash flow. And cash flow depends on claims getting paid. When eligibility verification is done correctly, the entire revenue cycle runs smoother.
Without it, the risk of claiming denials goes up sharply. Denied claims mean delayed payments. Delayed payments mean financial pressure on the practice. According to HHS.gov, billing errors and eligibility issues are among the leading causes of preventable revenue loss in US healthcare practices.
Eligibility verification is not just an administrative task. It is a financial protection strategy for every healthcare practice that wants to stay stable and grow.
How Claim Denials Connect Directly to Eligibility Errors
Claim denials do not usually come out of nowhere. Most of them trace back to an eligibility issue that was missed before the appointment. The insurance was inactive. The service was not covered. The patient had switched plans, and nobody knew.
Each of these situations is preventable. Proactive eligibility verification catches them before they become denials. When your team checks coverage details, confirms copays and deductibles, and flags any prior authorization requirements in advance, the number of claim rejections drops significantly.
For Texas healthcare organizations, where patient volumes are high and payer mixes are complex, this matters even more. The Texas Department of Insurance provides resources to help both providers and patients understand coverage rights and billing standards across the state.
Real Time Insurance Eligibility Verification Changes Everything
There was a time when verifying insurance meant calling the insurance customer service line, waiting on hold, and writing down benefits by hand. That process was slow, inconsistent, and left too much room for error.
Real-time insurance eligibility verification through platforms like Availity and TriZetto changed that entirely. Your staff can now pull a complete benefits summary in under two minutes. Services covered, copays, deductibles, coverage dates, and exclusions all appear instantly on one screen.
This does three things for your practice. It cuts down on administrative costs. It gives your team accurate information faster. And it reduces the manual errors that lead directly to claim denials and rework.
How Eligibility Verification Reduces the Burden on Your Staff
Ask any front desk coordinator what takes up most of their time and they will tell you it is chasing insurance information, fixing billing errors, and dealing with denied claims. All of that gets lighter when eligibility verification is automated and standardised.
When your team is not spending hours on hold with insurance customer service or resubmitting claims that should have been clean the first time, they can focus on what actually matters. Talking to patients. Coordinating care. Running the practice efficiently.
According to Healthcare.gov, understanding coverage details upfront is one of the most effective ways to reduce billing disputes between providers and patients across US healthcare services.
Effective Practices Every Texas Healthcare Practice Should Follow
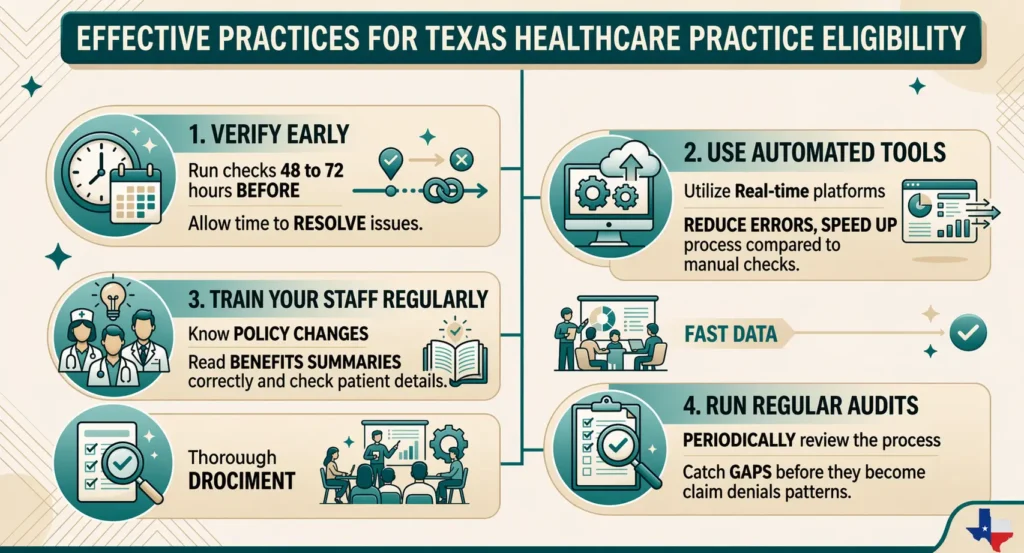
Getting eligibility verification right does not require a complete overhaul of how your practice operates. It requires consistency. Here are the practices that make the biggest difference.
Verify early. Do not wait until the day of the appointment. Run the check 48 to 72 hours before, so your team has time to resolve any issues.
Use automated tools. Real-time platforms reduce errors and speed up the process significantly compared to manual checks or insurance customer service calls.
Train your staff regularly. Insurance policies change. Your team needs to know how to read a benefits summary correctly and what to look for during patient registration.
Run regular audits. Periodically reviewing your eligibility verification process helps catch gaps before they turn into patterns of claim denials.
How Eligibility Verification Improves the Patient Experience
Patients do not want billing surprises. Nobody does. When a bill arrives weeks after a visit and it is far higher than expected, trust breaks down fast.
When your practice confirms insurance eligibility before the appointment and shares the results with the patient upfront, the whole experience changes. They know their copay before they arrive, understand what their plan covers. They are not caught off guard.
According to AHRQ, transparent financial communication in healthcare directly improves patient satisfaction scores and reduces the number of billings disputes a practice must manage. Patients who feel informed come back. They also refer to others.
Insurance eligibility verification is the process of confirming a patient’s active insurance coverage before delivering healthcare services. It checks copays, deductibles, covered services, and prior authorization needs. For Texas healthcare practices, this step prevents claim denials and keeps the medical billing process running smoothly from the very start.
Verifying insurance eligibility before every appointment protects your practice from unexpected claim denials and payment delays. It gives both your staff and your patients clarity on what is covered. For any healthcare organization in Texas, this single step directly strengthens revenue and reduces billing errors across the board.
Real time insurance eligibility uses electronic platforms like Availity to instantly pull a patient’s coverage details. Your team gets copays, deductibles, covered services, and exclusions in under two minutes. This replaces slow insurance customer service calls and significantly reduces the manual errors that lead to claim rejections in healthcare practices.
Eligibility verification should happen during patient registration, ideally 48 to 72 hours before the appointment. This gives your team enough time to resolve coverage issues before the patient arrives. Texas healthcare organizations that verify early report fewer claim denials and smoother patient experiences from check in through final billing.
Most claim denials in US healthcare practices trace back to eligibility errors. When your team confirms active coverage, copays, deductibles, and prior authorization requirements before the patient appointment, the chances of a rejection drop significantly. Proactive eligibility verification is the most effective way to protect your practice revenue every single day.
Yes. When patients know their insurance coverage details, copays, and financial responsibilities before their visit, there are no surprise bills afterward. This builds trust and loyalty. According to AHRQ, transparent billing communication directly improves patient satisfaction scores for healthcare services across Texas and the wider US healthcare system.
How Integrate Point Helps Texas Practices Get This Right
Managing eligibility verification across dozens of payers while running a busy practice is a lot to handle. That is where Integrate Point comes in.
Based in Texas, our team works directly with healthcare organizations across the state to build verification processes that are accurate, consistent, and scalable. We handle the complexity of confirming patient insurance coverage so your clinical team can stay focused on patient care.
From real time eligibility checks to full revenue cycle management, we bring the tools and the expertise to reduce claim denials, protect your revenue, and make the medical billing process work the way it should.
Contact Integrate Point today and let us take the administrative weight off your team.



