In the digital era, the healthcare sector, particularly medical billing, has emerged as a major target for cybercriminals. For all U.S. healthcare providers, from hospital systems to small and mid-sized clinics, medical billing is far more than a numbers game. It’s the critical juncture where finance meets patient privacy. It’s also about keeping patient information safe and staying on the right side of the HIPAA.
Ignoring these critical areas can lead to devastating consequences, from financial penalties to a complete erosion of patient trust.
If you’re running or managing a clinic in Dallas, TX, here’s what you need to know about cybersecurity in medical billing and how to stay HIPAA compliant while protecting your patients.
- Why Cybersecurity Matters in Medical Billing
- Common Cybersecurity Threats to Watch For
- HIPAA Compliance: More Than Just a Policy
- Ways to Keep Your Medical Billing Cybersecure
- Real-World Case Study: The Cost of Ignoring Cybersecurity
- Maintaining Trust and Compliance in the Digital Age
- Frequently Asked Questions on Medical Billing Security
- Conclusion
Why Cybersecurity Matters in Medical Billing
Medical Billing is a Hacker’s Goldmine (PHI & Finance)
Medical billing systems are a “goldmine” for cybercriminals because they contain a treasure trove of Protected Health Information (PHI) and financial data. Every step in the billing lifecycle, from sending a claim to processing an Explanation of Benefits (EOB), involves handling sensitive PHI. This makes your practice a prime target.
What makes a medical record so valuable?
- A single stolen medical record can fetch a high price on the black market.
- It provides a complete identity package: names, SSNs, insurance details, diagnosis codes, and payment information.
Small and mid-sized clinics are especially vulnerable. Hackers know these practices often lack enterprise-grade IT protections.
The Cost of Non-Compliance:
Even a minor data breach can trigger HIPAA fines ranging from $100 to $50,000 per violation. A ransomware attack can lock you out of your data overnight.
Common Cybersecurity Threats to Watch For
Cybercriminals employ increasingly sophisticated methods. Here are some of the most common threats targeting healthcare billing:
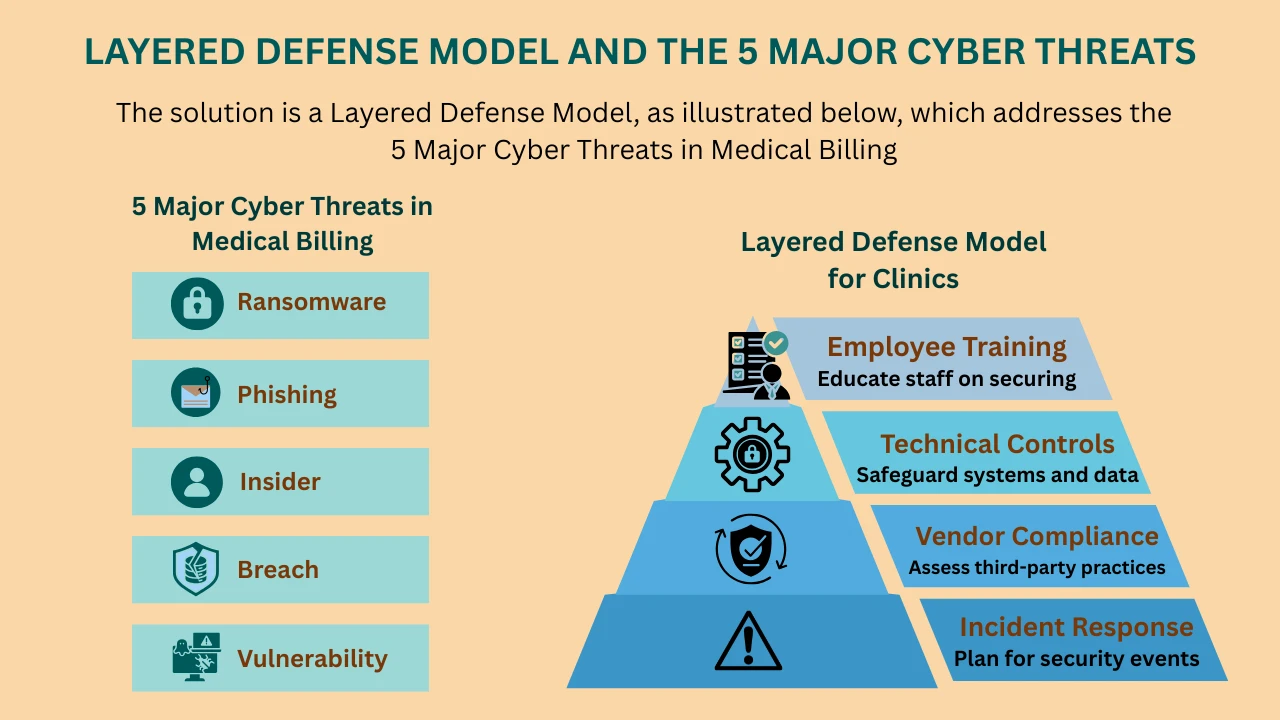
- Ransomware: Malware encrypts your billing and EHR systems, blocking access until a ransom is paid. Even after payment, data may not be fully restored, and downtime can cost your clinic thousands per day.
- Phishing Attacks: Deceptive emails or messages designed to trick staff into revealing login credentials or downloading malware, leading to unauthorized system access.
- Insider Threats: Employees, either maliciously or negligently, misusing their authorized access to sensitive data. This can include accidental data exposure or intentional theft.
- Data Breaches: Unauthorized access to or disclosure of PHI, often resulting from vulnerabilities in systems or human error.
- Vulnerabilities in Systems and Software: Exploitable weaknesses in billing platforms, EHR systems, or even third-party vendor software that open the door for exploitation.
HIPAA Compliance: More Than Just a Policy
The Health Insurance Portability and Accountability Act (HIPAA) establishes federal guidelines to ensure the confidentiality and security of protected patient health information.
In medical billing, HIPAA compliance means safeguarding PHI throughout the entire billing lifecycle – from eligibility verification and claim submission to payment posting and patient statement processing. And while compliance might feel like a checklist item, it’s truly the foundation of patient trust and legal protection.
Key HIPAA Rules Impacting Medical Billing
- The Privacy Rule: Outlines how Protected Health Information (PHI) may be used and disclosed. Only authorized personnel should access billing records containing patient data.
- The Security Rule: Imposes administrative, physical, and technical safeguards for Electronic Protected Health Information (ePHI). Notably, the Office for Civil Rights (OCR) has proposed updates to the HIPAA Security Rule for 2025, which will make many safeguards mandatory, intensifying scrutiny.
Billing systems must meet HIPAA’s Security Rule standards, which include:- Administrative safeguards (like training and audits)
- Physical safeguards (like access to servers or file storage)
- Technical safeguards (like encryption, password protections, and data monitoring)
- The Breach Notification Rule: Requires covered entities and business associates to notify affected individuals and the HHS OCR in the event of a breach.
While HIPAA compliance is a legal requirement with significant penalties for non-compliance, it’s crucial to understand that it provides a framework, not a real-time defense system. Hackers don’t care about your compliance forms; they care about vulnerabilities.
Ways to Keep Your Medical Billing Cybersecure
While HIPAA compliance is essential, it’s not foolproof. Hackers don’t care about checklists; they care about vulnerabilities.
That’s why every clinic needs a cybersecurity strategy that blends compliance with active defense. A proactive, layered approach is essential for small clinics to protect patient data and maintain tight HIPAA compliance.
Layered Approach
- Conduct Regular Risk Assessments: Periodically identify potential weak spots and threats to your ePHI. This helps you understand where your data is most at risk.
- Invest in Comprehensive Employee Training: Human mistakes continue to be the root cause of breaches. Regular, mandatory training on
- Identifying phishing attempts,
- Pro per data handling,
- Secure communication methods
- Report suspicious activity immediately
- Implement Strong Technical Safeguards:
- Encryption: Encrypt all PHI, “at rest” (stored information) and “in transit” (data in motion).
- Multi-Factor Authentication (MFA): Require MFA for all system access to add an extra layer of security beyond just passwords.
- Access Controls: Use role-based access, allowing access only by authorized staff for PHI pertinent to their job responsibilities.
- Firewalls & Antivirus Software: Maintain up-to-date firewalls and antivirus/anti-malware solutions.
- Secure Networks: Ensure your clinic’s Wi-Fi and internal networks are secure and segmented.
- Implement Physical Security Measures: Secure physical access to your information. This includes securing servers, workstations, and paper records in locked cabinets or restricted areas.
- Vet Your Business Associates (BAs): Any third-party vendor that handles your PHI (including medical billing companies, EHR providers, IT support) must be HIPAA-compliant and sign a Business Associate Agreement (BAA). This commits them legally to safeguard your patient’s information.
- Develop an Incident Response Plan: Have a clear, well-rehearsed plan in place for how your clinic will respond in the event of a suspected or confirmed data breach. Your team should know:
- Whom to notify
- How to isolate affected systems
- What documentation is needed for the OCR
- Regular Audits and Monitoring: Continuously monitor your systems for unusual activity and conduct regular internal and external audits at least once a year, to ensure ongoing compliance and identify new vulnerabilities.
Real-World Case Study: The Cost of Ignoring Cybersecurity
A small cardiology clinic in Houston faced a ransomware attack in 2024 that froze access to over 12,000 patient records.
The clinic had no recent backups, no MFA, and had skipped annual risk assessments.
The fallout was severe:
- $50,000 fine for HIPAA non-compliance
- $200,000 in lost revenue due to downtime
- 23% patient drop due to loss of trust
By contrast, another Dallas-based clinic that partnered with a HIPAA-compliant billing vendor had zero downtime and 99% recovery after a similar attack — thanks to encrypted backups, regular audits, and proactive monitoring.

Maintaining Trust and Compliance in the Digital Age
Patients trust you not only with their health but with their most personal information. A single data breach can damage trust irreparably.
Protecting PHI is not just a regulatory checkbox; it’s an ethical responsibility. Clinics that actively invest in cybersecurity build stronger patient relationships, reduce risks, and project a professional image that inspires confidence.
Frequently Asked Questions on Medical Billing Security
1. Does HIPAA compliance automatically mean I’m protected from hackers?
No. HIPAA provides a framework and legal requirements, but it is not a real-time defense system. Hackers don’t care about compliance forms; they care about vulnerabilities. You need to blend compliance with an active, layered defense strategy.
2. What is the single most effective way to protect our ePHI?
Implementing a strong Multi-Factor Authentication (MFA) policy for all system access, combined with comprehensive, regular Employee Training (human error is the root cause of many breaches).
3. How often should we conduct a risk assessment?
You should periodically identify weak spots and threats to your ePHI, with at least one full internal and external audit conducted annually.
Conclusion
Cybersecurity in medical billing goes beyond technology; it’s the backbone of patient trust, operational stability, and financial wellbeing. With a proactive, multi-layered defense and strict HIPAA compliance, clinics can protect confidential information, reduce risks, and succeed with confidence in the evolving healthcare environment.
At Integrate Point, we help Dallas based medical practices like yours simplify compliance and secure sensitive billing data. From system audits and staff training to selecting HIPAA-compliant tools, we support your clinic at every step.
Take Action Now: Fortify Your Clinic Against Cyber Threats
Don’t wait for a data breach to expose the vulnerabilities in your system. The cost of proactive defense is always lower than the cost of a HIPAA fine, lost revenue, and patient distrust. Ready to achieve tight HIPAA compliance and impenetrable data security? Schedule your FREE Cybersecurity & HIPAA Risk Assessment with Integrate Point and fortify your billing operations today!




Great article! It really highlights the critical intersection of cybersecurity and patient data protection in medical billing. This got me thinking about a related aspect of patient trust and data privacy: the handling of sensitive mental health information.
I was recently researching the challenges foreign visitors face when accessing mental health care in the U.S., particularly regarding costs and data security protocols. I came across a detailed guide that explains this complex system. Sorry for dropping a link here, but it really helps illustrate the specific point I’m trying to make about the importance of transparent information handling. The page at https://pillintrip.com/fr/article/mental-health-usa-what-foreign-visitors-need-to-know-about-access-and-costs provides a breakdown of access barriers and pricing, which seems like a massive data privacy and security concern in itself.
My question is: For a medical billing provider, how do you see the cybersecurity protocols for medical billing (like those you outlined for PHI) extending to protect the financial and access information of patients seeking sensitive care, like mental health treatment? Are there additional layers of security or compliance considerations when processing bills for such sensitive services, especially for vulnerable populations like international patients who might be less familiar with the U.S. system?
Thank you for the thoughtful comment and bringing in an important dimension to the discussion: the protection of sensitive information on mental health, most especially for an international patient who might first encounter the U.S. healthcare system. You are absolutely right that mental health billing carries additional sensitivity compared with usual PHI.
At Integrate Point, all core HIPAA and cybersecurity safeguards apply, but mental health-related billing often requires additional layers of protection. We implement stricter access controls, enhanced audit monitoring, and data segmentation practices in order to ensure that only the minimum necessary information is accessible to authorized staff. We also stay compliant with stricter confidentiality regulations, including relevant state laws when applicable.
So, transparency is especially important with international and vulnerable patient groups, so we encourage clear communication around what data is collected, how it is used, and how it remains protected.
Awesome blog.
We are glad that you found our blog awesome.