A patient leaves their primary care appointment with a referral slip in hand. The doctor has done their part. But what happens next is where things quietly fall apart. The patient tries to book. The specialist’s office needs records that nobody sent. Insurance has not been verified. Prior authorization was never requested. Three weeks later the appointment still has not happened, and nobody in your clinic even knows.
That is not a patient problem. That is a specialist referral management problem. And for healthcare managers and clinic administrators across Texas, it is one of the most expensive and avoidable sources of revenue loss and patient dissatisfaction in the entire practice.
This blog walks through exactly where the referral process breaks down, what the data shows, and what healthcare managers can do right now to fix it.
- Why the Referral Process Breaks Down Before It Even Starts
- The Real Numbers Behind Specialist Referral Problems
- What Healthcare Managers Are Actually Dealing with Every Day
- Five Things Healthcare Managers Can Do Right Now
- 1. Standardize Your Referral Intake with a Dedicated Referral Coordinator
- 2. Automate Insurance Verification Before Every Appointment
- 3. Use Automated Patient Reminders to Reduce No Show Rates
- 4. Integrate Records Through EHR Integration and Health Information Exchange
- 5. Close the Referral Loop with Structured Follow Up
- What Patients Need from the Referral Process
- Frequently Asked Questions
Why the Referral Process Breaks Down Before It Even Starts
Most referral failures do not happen because of bad intentions. They happen because nobody owns the process from end to end. Information travel by fax. Staff manually chase records. Patients get a name and a number and are left to figure out the rest themselves.
According to AHRQ, care coordination gaps including incomplete referral follow through are among the leading causes of preventable complications and avoidable costs across US healthcare systems. The referral that nobody tracked is not just a revenue problem. It is a patient safety problem.
For clinic administrators, the referral process represents one of the highest concentration points of operational risk in the entire practice. Getting it wrong costs money, costs patients, and costs your reputation.

The Real Numbers Behind Specialist Referral Problems
Before fixing something, you need to see it clearly. Here is what the research shows where specialist referral management is failing across US healthcare practices right now.
According to the Medical Group Management Association, healthcare organizations implementing structured referral workflows report a 35% improvement in appointment fulfillment rates. Practices using automated systems reduce referral processing time from 47 minutes down to 12 minutes per referral.
The Journal of Healthcare Management reports that multi touch patient communication increases specialist appointment attendance by 28%. Practices with pre visit patient education report 40% fewer clarification calls on the day of the appointment.
According to HIMSS, 67% of specialist delays are directly attributed to missing prior medical records. Only 23% of specialist practices currently have direct EHR integration with referring practices. That gap is where referral leakage lives.
What Healthcare Managers Are Actually Dealing with Every Day
Understanding the operational reality is the first step toward fixing it. Here is what clinic administrators across Texas report as their biggest referral pain points.
Fragmented Communication Between Practices
Referral information arrives in every format imaginable. Fax, email, patient hand delivery, or sometimes just what the patient remembers from their last appointment. Each format requires manual processing. Each one creates opportunities for critical information to get lost before the specialist ever sees the patient.
The average time spent on referral reconciliation is 15 to 30 minutes per referral. In a busy clinic handling 20 or more referrals a week, that adds up to hours of staff time that could be spent on patient care.
Insurance Verification and Prior Authorization Gaps
Manual insurance verification workflows consume up to 30% of front desk staff time in practices without insurance verification software. When prior authorization requirements are missed, appointments get delayed by two to three weeks. Patients find out about the barrier only after they have already tried to confirm their appointment. By then the frustration has already set in.
According to CMS, prior authorization issues are among the most cited reasons for specialist appointment delays across US Medicare and Medicaid populations. This is a systemic problem with a systemic solution.
High No Show Rates Draining Revenue
Specialist practices report 25 to 30% no show rates for new patient visits. Each missed appointment costs between $300 and $800 depending on specialty. Beyond the direct revenue loss, no shows create underutilized clinical time, reduce availability for other patients, and add rescheduling work back onto already stretched administrative teams.
Most of these no shows are preventable. Patients do not show up because they did not understand what to bring, did not know where to go, or simply forgot. These are not complex problems. They are communication problems.

Five Things Healthcare Managers Can Do Right Now
These are not theoretical improvements. They are operational changes that clinics across Texas are implementing today and seeing measurable results within months.
1. Standardize Your Referral Intake with a Dedicated Referral Coordinator
The single biggest structural change a clinic can make is assigning a dedicated referral coordinator to own the process from start to finish. This person is responsible for making sure every referral goes out with complete clinical information attached; every prior authorization is requested before scheduling, and every record transfer is confirmed before the patient’s appointment.
According to AHRQ, practices with dedicated referral coordination roles report significantly fewer administrative callbacks and measurably higher referral completion rates compared to those relying on general front desk staff to manage referrals alongside other duties.
Standardize the intake form. Make sure it captures the clinical reason, urgency level, relevant medical history, and any imaging or lab results that need to accompany the referral. Make it a non-negotiable checkpoint before any referral leaves the practice.
2. Automate Insurance Verification Before Every Appointment
Insurance verification software eliminates the manual process of calling payers to confirm coverage and identify prior authorization requirements. When this step is automated, staff get instant confirmation of what is covered, what the patient owes, and whether pre-approval is needed before the appointment is even confirmed.
This single change eliminates up to 70% of pre-appointment phone calls and reduces cancellations due to insurance surprises by 30%. Patients are informed of their copay and coverage details before they arrive. No surprises. No last-minute cancellations.
The impact on your healthcare revenue cycle is direct. Fewer cancellations mean fewer empty slots. Fewer prior auth misses mean fewer delayed payments and denied claims.
3. Use Automated Patient Reminders to Reduce No Show Rates
The research is clear about this. Automated patient reminders sent at multiple points before the appointment significantly reduce no show rates across specialist practices.
The most effective approach uses automated appointment reminders at three points: two weeks before, one week before, and two days before the appointment. Each message includes specific details about what to bring, where to go, how to prepare, and who to call with questions.
According to the Journal of Healthcare Management, practices using automated reminders reduce no shows by 20 to 35%. For a specialist practice losing $400 per no show slot, even a 20% reduction across 100 monthly referrals represents significant recovered revenue every single month.
Automated patient reminders also reduce the anxiety that leads to cancellations. When patients feel informed and prepared, they show up.
4. Integrate Records Through EHR Integration and Health Information Exchange
One of the most impactful and underused tools available to healthcare managers today is health information exchange. HIE allows your practice to pull records directly from external EHR systems without requiring the patient to hand carry documents or staff to chase faxes.
EHR integration with referring practices means that by the time the patient arrives for their specialist visit, the specialist already has their imaging, lab results, and clinical notes loaded and reviewed. Visit time shortens by 15 to 20 minutes. Redundant testing drops dramatically. And the patient experience improves because they are not being asked to repeat information, they already gave their primary care doctor.
According to HealthIT.gov, healthcare organizations using health information exchange report a 45% reduction in redundant testing and significantly faster time to diagnosis for referred patients. Healthcare interoperability is no longer a future goal. It is an available solution that clinics are implementing right now.
How EHR Integration and HIE Transform the Specialist Visit
| Without EHR Integration | With EHR Integration and HIE |
| Patient hand carries records or forgets them | Records pulled automatically before appointment |
| Staff chase faxes from referring practice | Direct data exchange between systems |
| Specialist reviews incomplete history | Full clinical context available at visit |
| Duplicate tests ordered for missing results | Redundant testing reduced by up to 45% |
| Visit runs 15 to 20 minutes longer | Shorter visit, faster diagnosis |
| Referring provider rarely gets notes back | Closed loop referral completed automatically |
5. Close the Referral Loop with Structured Follow Up
A closed loop referral means that when a patient sees the specialist, the specialist’s findings, recommendations, and next steps come back to the referring provider within 24 to 48 hours. The loop is complete. The care is coordinated. The patient is not left navigating between two practices that are not talking to each other.
Referral follow up is the step that most clinics skip because it feels like the specialist’s responsibility. In practice, if nobody is tracking it, nobody is doing it. Your referral coordinator should be monitoring every open referral and following up when communication has not come back within the agreed window.
According to HHS.gov, care continuity is directly linked to patient trust, reduced readmission rates, and improved long term health outcomes. Closing the referral loop is not just a good administration. It is a good medicine.
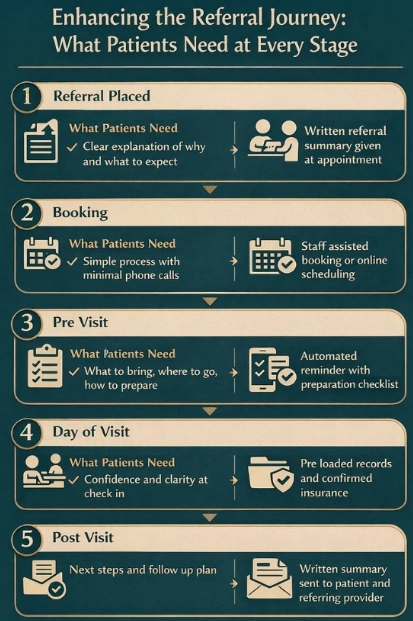
What Patients Need from the Referral Process
Healthcare managers sometimes focus entirely on the operational side and forget that the patients experience is the other half of the equation. When patients are confused, unprepared, or anxious, they do not show up. When they do not show up, everything else fails.
The fix is straightforward. Give every patient a clear written summary when the referral is placed. Tell them why they are being referred, what the specialist will evaluate, what to bring, and what to expect. Make the booking process as simple as possible. Follow up if they have not booked within a week.
According to AHRQ, patients who receive structured pre-referral education report significantly lower anxiety levels and measurably higher specialist appointment completion rates. Informed patients show up. Confused patients do not.
Frequently Asked Questions
Specialist referral management is the end-to-end process of sending a patient from a primary care provider to a specialist, ensuring records are transferred, insurance is verified, appointments are completed, and findings return to the referring provider. When managed well, it protects both care continuity and healthcare revenue cycle performance for Texas clinics.
A referral coordinator owns the entire referral journey from intake to closed loop follow up. They ensure clinical information is complete before scheduling; prior authorizations are secured on time, and specialist findings return to the referring provider. Practices with dedicated referral coordinators report measurably higher referral completion rates and fewer administrative errors.
Automated patient reminders sent at two weeks, one week, and two days before the appointment give patients the information they need to prepare and show up. When patients know what to bring, where to go, and what to expect, cancellation rates drop significantly. Research shows automated reminders reduce no shows by 20 to 35% across specialist practices.
A closed loop referral means the specialist’s findings, recommendations, and next steps to return to the referring provider within 24 to 48 hours of the visit. Without this, care becomes fragmented, and patients fall through the gaps. Closing the loop protects care continuity, reduces unnecessary repeat visits, and strengthens the relationship between referring and specialist practices.
Referral leakage happens when patients see out of network specialists after a referral is placed. The revenue from those visits does not return to your system. For Texas clinics, even a modest leakage rate represents significant annual losses. Structured specialist referral management with proper tracking and follow up is the most effective way to close those gaps.
How Integrate Point Helps Texas Clinics Fix Specialist Referral Management
At Integrate Point, we work with healthcare managers and clinic administrators across Texas to build referral management systems that actually close the loop. From referral coordinator support to insurance verification software integration, EHR connectivity, and automated patient reminder workflows, we handle the operational complexity so your team can focus on care.
We understand what Texas clinics are dealing with because we work inside these systems every day. Our team helps you identify your highest leakage points, automate your verification workflows, and build the structured follow up processes that keep your healthcare revenue cycle healthy.
Book a consultation with our team today. We will walk you through the top three referral fixes that deliver the fastest results for practices your size.



